Cyborgs are real and they’re in trouble. They are the millions of people around the world who live with pacemakers and insulin pumps implanted in their augmented bodies.
But when things go wrong with their devices, cyborgs are victims of an extremely prosaic issue: they have pathetic consumer protections, even when the device in question is life-sustaining. Between 2008 and 2018, more than 80,000 deaths and 1.7 million injuries worldwide were linked to the failure of various medical implants (things like prosthetic hips, spinal stimulators, or cardiac devices).
The reason? For-profit healthcare organizations have a history of prioritizing bottom lines over bioethics. When promising quality products threatens a company’s financial standing, patients are quickly abandoned. Stories like these are very common: Second Sight Medical Products terminated bionic eye user Barbara Campbell’s vision while she transferred subways in the middle of a New York City station. Nuvectra went bankrupt and orphaned their spinal-cord stimulators in 3,000 patients. Boston Scientific ignored a known defect in their pacemakers that resulted in electrical arcing, and at least one patient died due to their cardiac device short-circuiting while inside of their chest.
Due to high costs, obsolescence, and design flaws, patients need devices that actually last a lifetime. Pacemaker failures specifically are often the result of complications from their lithium-ion battery. Because of their checkered history, scientists are seeking new ways to harvest energy to power devices that don’t rely on batteries. For an experimental lab in South Korea, that means banking on our own organs for electricity, a radical move that could challenge the fundamental paradigms of patient’s rights laws. Their recent Advanced Materials publication investigates whether pacemakers can be powered by the expansion and contraction of the wearer’s own heart.
Piezoelectric materials can convert mechanical force into an electric charge. Engineers implement this type of hardware to harvest compression on pavement beneath heavy vehicles, to harvest tidal wave energy off the coast of Oahu, Hawai’i, and even to harvest body movement within a T-shirt. The lab at Hanyang University in Seoul led by Seon Jeong Kim put those circuits outside the heart.
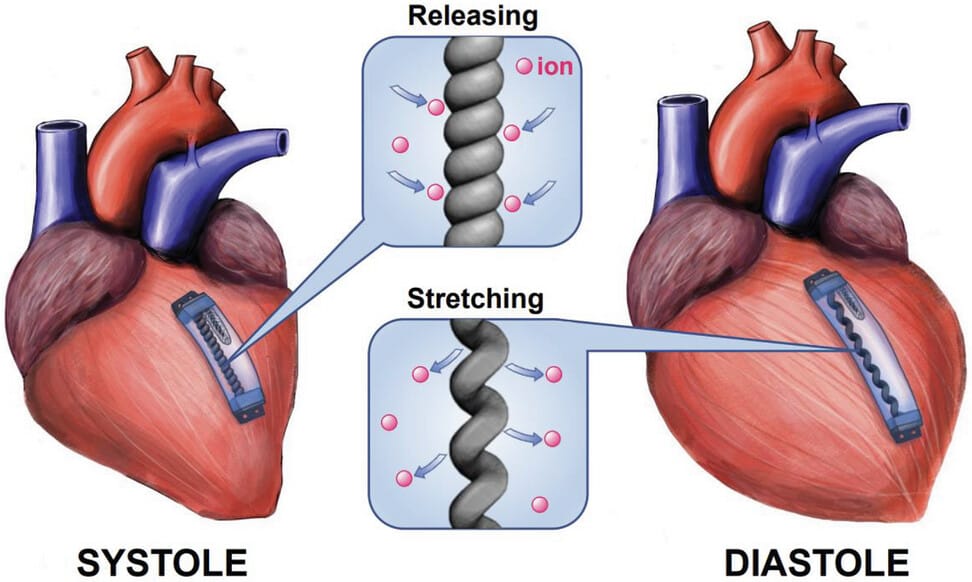
The science behind this comes from a 2017 paper about nanoscopic graphene. Cylindrical sheets of graphene are woven together, coiled, and soaked in saltwater to form a tangible, yarn-like structure called Twistron. Pulling and compressing Twistron generates a current. It currently has the highest power output in the widest frequency range of any other known mechanical energy harvester. It’s as though you could power a lightbulb by stretching an attached bungee cord. The basic design of yarn soaked in brine is thought to be much simpler and more reliable than batteries, lowering risk for patients. In order to power an organ in the human body, all you have to do is install it somewhere capable of tugging.
The surface of the heart changes shape during a heartbeat. Blood fills the ventricles, increasing the heart's volume, then pumps out to the rest of the body, reducing the heart’s volume before the cycle restarts. In the swelled state, the heart muscle could hypothetically tug on a piezoelectric material. For this approach, the left ventricle has the most promise. It’s the heart's main pumping chamber, with the thickest muscular walls (about as thick as a standard matchbox) and highest pressure buildup to circulate blood effectively. To see whether the left ventricle tugs enough to trigger Twistron’s piezoelectricity, the authors tested their heart-powered heart powerer, which they call the Twistron Energy Cell Harvester, or TECH.
To test the TECH, a water-filled balloon with a motor attached acts enough like a left ventricle for the experiment’s purposes. The authors programmed different rotation angles and speeds into the motor to mimic the heart’s complex strain. When beating at 60 beats per minute, the TECH produced 0.338 micro Joules of energy per cycle. For reference, the minimum amount of energy for a human heart to pulse is 0.377 micro Joules. Just by harvesting the physical movement of the (balloon mimicking a) heart, the TECH could recreate the heart’s approximate energy input.
The authors put the devices longevity to the test and conducted 50,000 stretch-and-release cycles, showing that TECH retained 94% of its energy output (the heart beats double that many times in a single day). But, because TECH relies on a completely reversible mechanical-electrochemical reaction, the authors expect TECH’s lifetime to be semi-permanent, much longer than that of a lithium-ion battery.
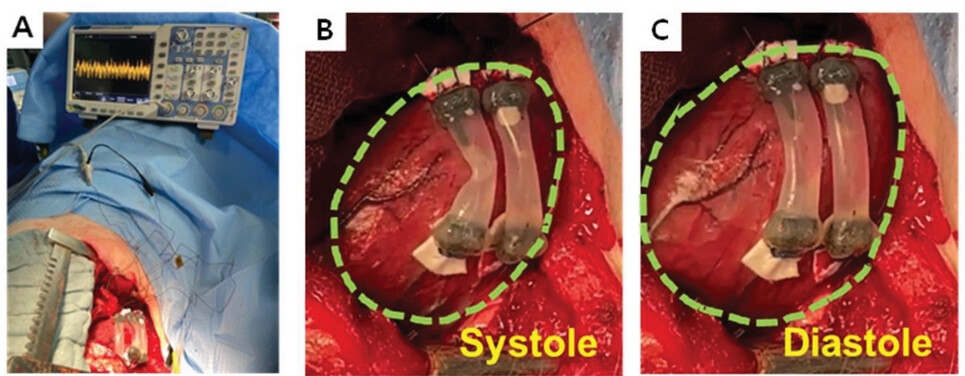
The first living organism to test the performance of TECH was a German Landrace pig. The authors sutured the device to the apex of the pig’s left ventricle. In its current form, a singular TECH is not able to generate the necessary voltage, so they sutured four serially connected devices. Its dimensions are relatively small (about the size of a grape), though four of them do take up much of the cardiac surface, so TECH still needs to be made smaller.
The true test took place when the authors performed an atrioventricular ablation, meaning they gave the pig cardiac arrest and then used the TECHs to restart the heart. They located where the heartbeat restarted with 3D anatomical ultra-high-density mapping. Amazingly, the mapping showed that the heart beat originated at the site of the TECH, meaning that the TECH harvested mechanical energy from the heart, converted it into electrical impulses, which it then emitted to excite the heart when it flat-lined.
Although we may become more and more cyborg-like, patients cannot be treated like old machines. For people with arrhythmias, the performance of their pacemakers is a matter of survival. Despite being invented over 60 years ago, the device's design is still not foolproof. Lithium-ion batteries are prone to depletion and hazards. The once futuristic biomedical device has become ordinary. It needs more innovation to bring its maintenance plans into the future. Scientists do not need to manufacture devices with higher degrees of complexity, which likely come with high maintenance needs as well. Instead, using the body itself as a source of inspiration and of power allows for more harmony and longevity. Implant designs that integrate seamlessly into our body’s natural roles allow for more intuitive and more human-centered technologies.
These bioethical objectives are necessary for a new era of patient rights. As we enjoy the fruits of biomedical successes, let’s not forget the dignity of the patients who depend on not only technology but on humanity.